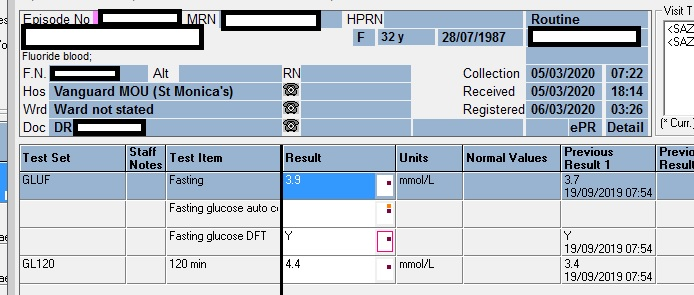
Falsely decreased glucose
| HOSP # | WARD | Antenatal Clinic | |
| CONSULTANT | Dr Heleen Vreede | DOB/AGE | 30y Female |
Abnormal Result
Glucose of < 0.1 mmol/L in a healthy individual being compos mentis.
Presenting Complaint
The patient is following up for routine check-up concerning possible hyperglycemia.
History
The mother is a known diabetic on treatment.
Examination
N/A
Laboratory Investigations
| Glucose at 11h00 | <0.1 mmol/L |
| Glucose at 14h00 | 1.5 mmol/L |
| Glucose at 20h00 | 2.6 mmol/L |
| Glucose at 06h00 (next morning – the day on which bloods were sent to the laboratory) | 6.2 mmol/L |
Other Investigations
| Glucose at 11h00 | 0.8 mmol/L |
| Glucose at 14h00 | 2.6 mmol/L |
| Glucose at 20h00 | 2.1 mmol/L |
| Glucose at 06h00 (next morning – the day on which bloods were sent to the laboratory) | 5.7 mmol/L |
The condition of the collection tubes were confirmed. All were taken in the correct collection tubes (Sodium Fluoride tubes) and appears to be correctly labelled.

Final Diagnosis


The conclusion from above findings are the following:
- Not enough NaF was present in the sample to adequately inhibit glycolysis, enabling a falsely decreased glucose reading in the older samples (>12 hours old).
- The patient wasn’t aware that the powder should stay in the tube when blood is collected, hence discarded the powder before taking her capillary blood samples.
Take Home Message
- Microtainer (R) specimen containers can be identified without the caps by the colour of the writing on the outside of the tube (in this case grey – the same colour as the cap).
- The presence of the correct collection tube does not equal the presence of the additive.
- Attention to detail is necessary to solve cause and effect in some cases.
- In this case the nursing staff in the Antenatal clinic was informed about the powder in the collection tubes which should not be discarded. The nurse whom I spoke to was completely unaware that the powder in the collection tube served any function.
- Glucose measurement from capillary blood samples, as in this case, can likely be inaccurate due to many possible pre-analytical (or analytical) reasons. It is however still likely a valid alternative to a resource-constrained setting, especially in South Africa, where patients cannot afford their own glucometers or where there are shortages of handheld glucometers, or more importantly, glucose measuring sticks (or cartridges).